The Touchless AI Operating System for Revenue Cycle
Healthcare loses $262B annually to billing inefficiency
Manual claims processing, preventable denials, and slow appeals drain revenue from health systems. The average hospital writes off 3-5% of net revenue to administrative waste.
Denial Rate
20%
12.4%
Days in AR
52 days
38 days
Cost to Collect
3.4%
2.8%
Automation Rate
12%
67%
Net Collection
Manual
96.8%
Write-Off Rate
2.0%
1.2%
Every step of the revenue cycle, automated
Purpose-built AI agents handle each phase with superhuman accuracy and speed.
Autonomous Agent Fleet
6 specialized AI agents -- DenialBot, PostBot, CodeBot, EligBot, UnderpayBot, and CDI-QueryBot -- process claims end-to-end with zero human touch.
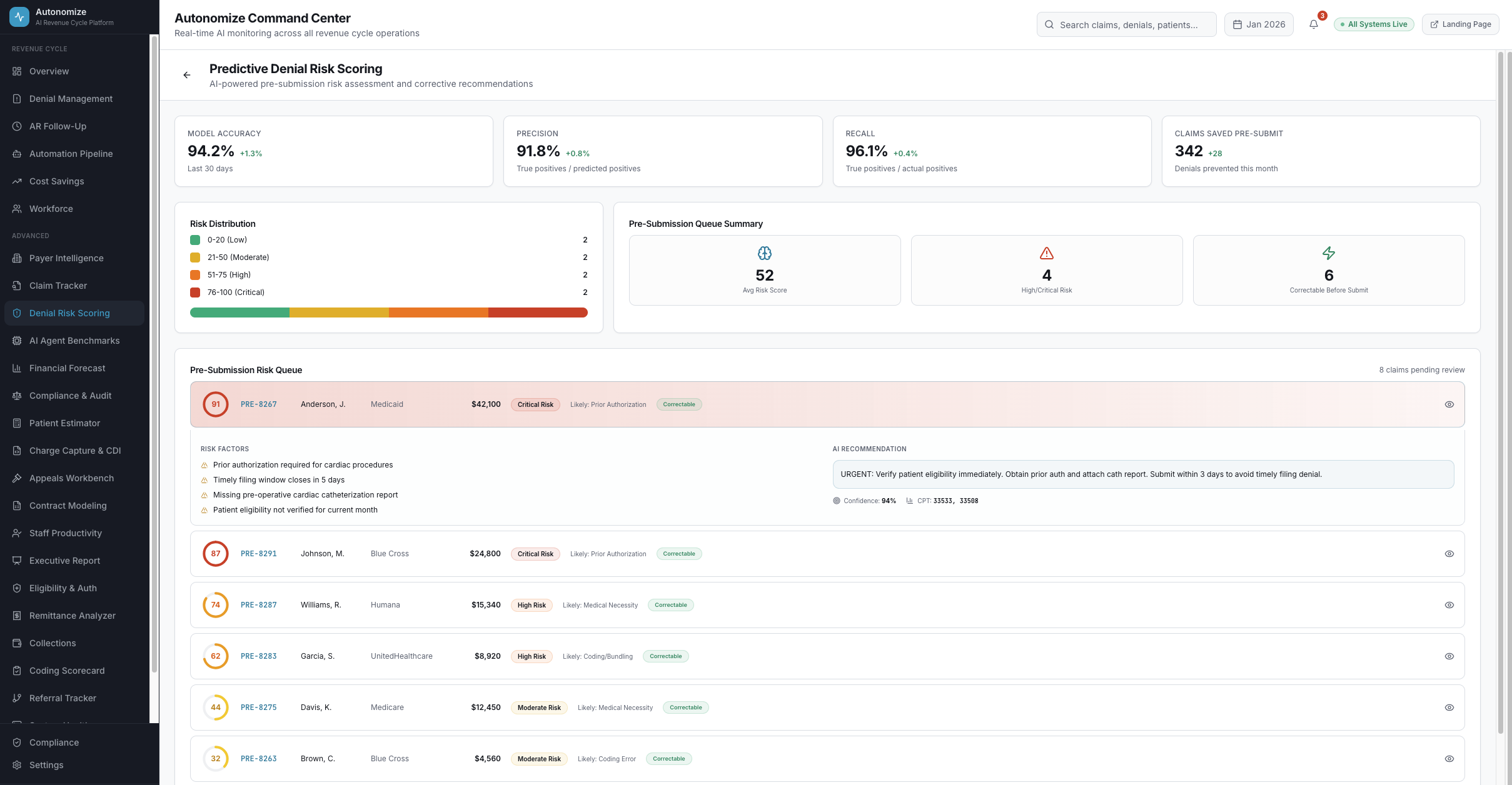
Pre-Submission Risk Scoring
Every claim scored before submission. 94.2% accuracy in predicting denials with real-time corrective recommendations before the claim leaves the building.
ADAA Denial Engine
Autonomous Denial & Appeal Agent ingests EDI 835s, triages by category, retrieves clinical evidence via FHIR RAG, and files legally-defensible appeals.
Real-Time Claim Tracking
End-to-end visibility: which bot touched it, what action was taken, current payer response, and full audit trail. Every claim, every step.
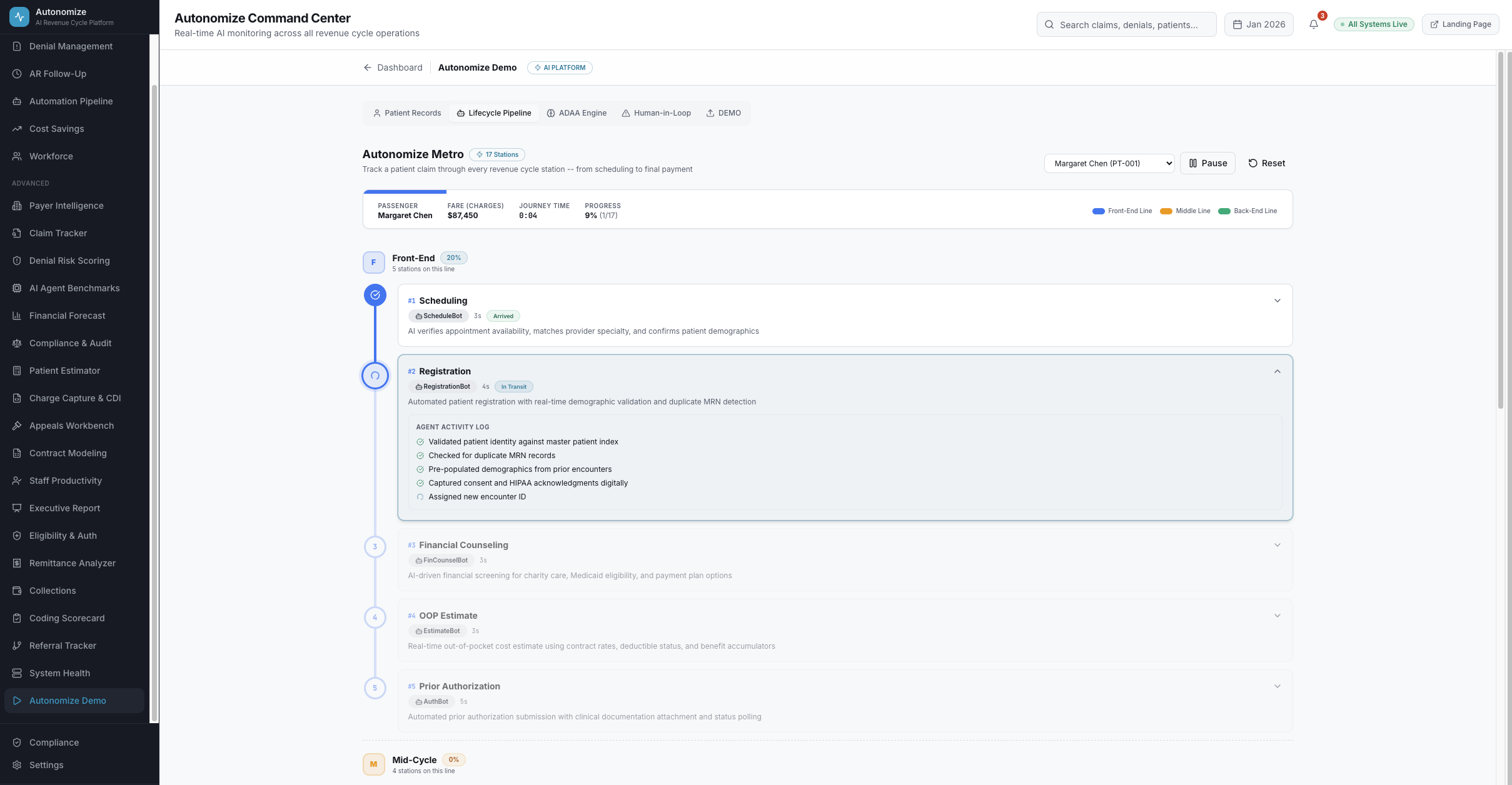
17-Station Pipeline
Tube-map visualization of the complete revenue cycle -- from scheduling to final QA, each station runs its own AI agent autonomously.
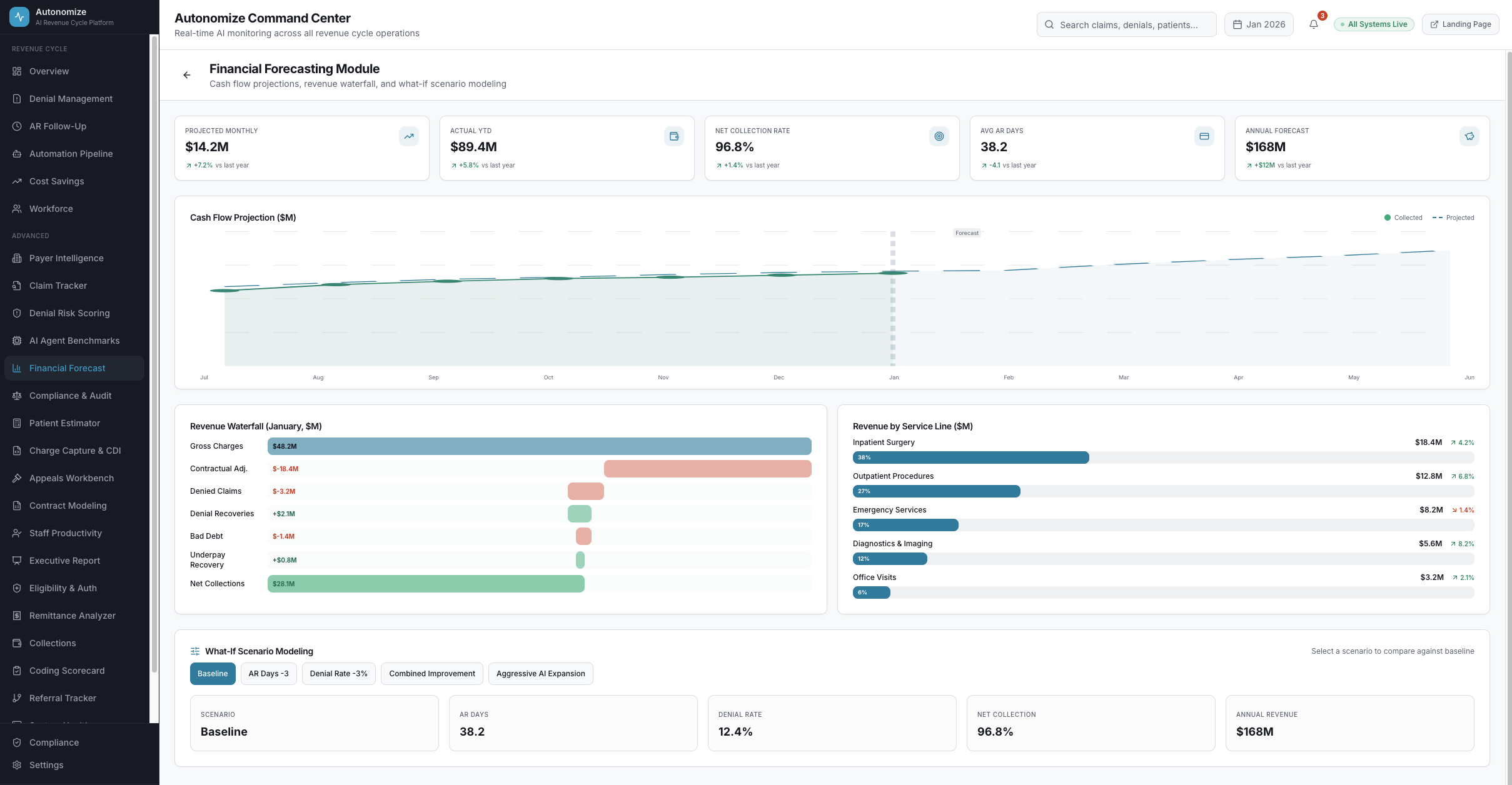
Financial Forecasting
Cash flow projections, revenue waterfalls, and what-if scenario modeling showing exactly how AI automation impacts your bottom line.
Watch the numbers move
Denial trend declining 35% over 6 months. Automation pipeline processing 4,210 claims per day.
Denial Trend (6-Month)
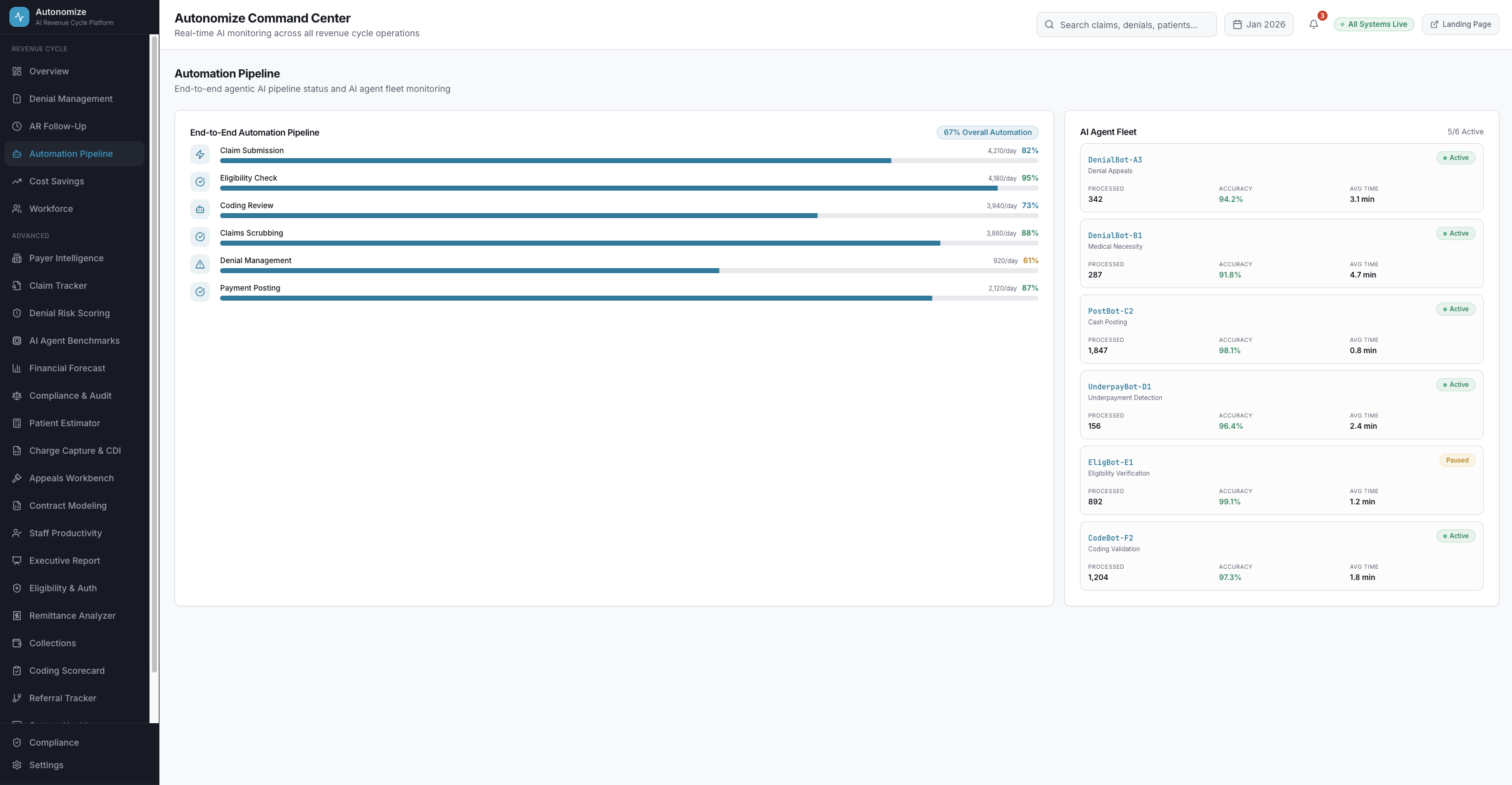
-35% reductionAutomation Pipeline
67% overall automation17 AI stations. One autonomous pipeline.
Inspired by the London Underground -- every station a claim passes through is powered by a dedicated AI agent. Select a patient, hit Depart, and watch the entire journey in real-time.
Front-End
5 stationsMid-Cycle
4 stationsBack-End
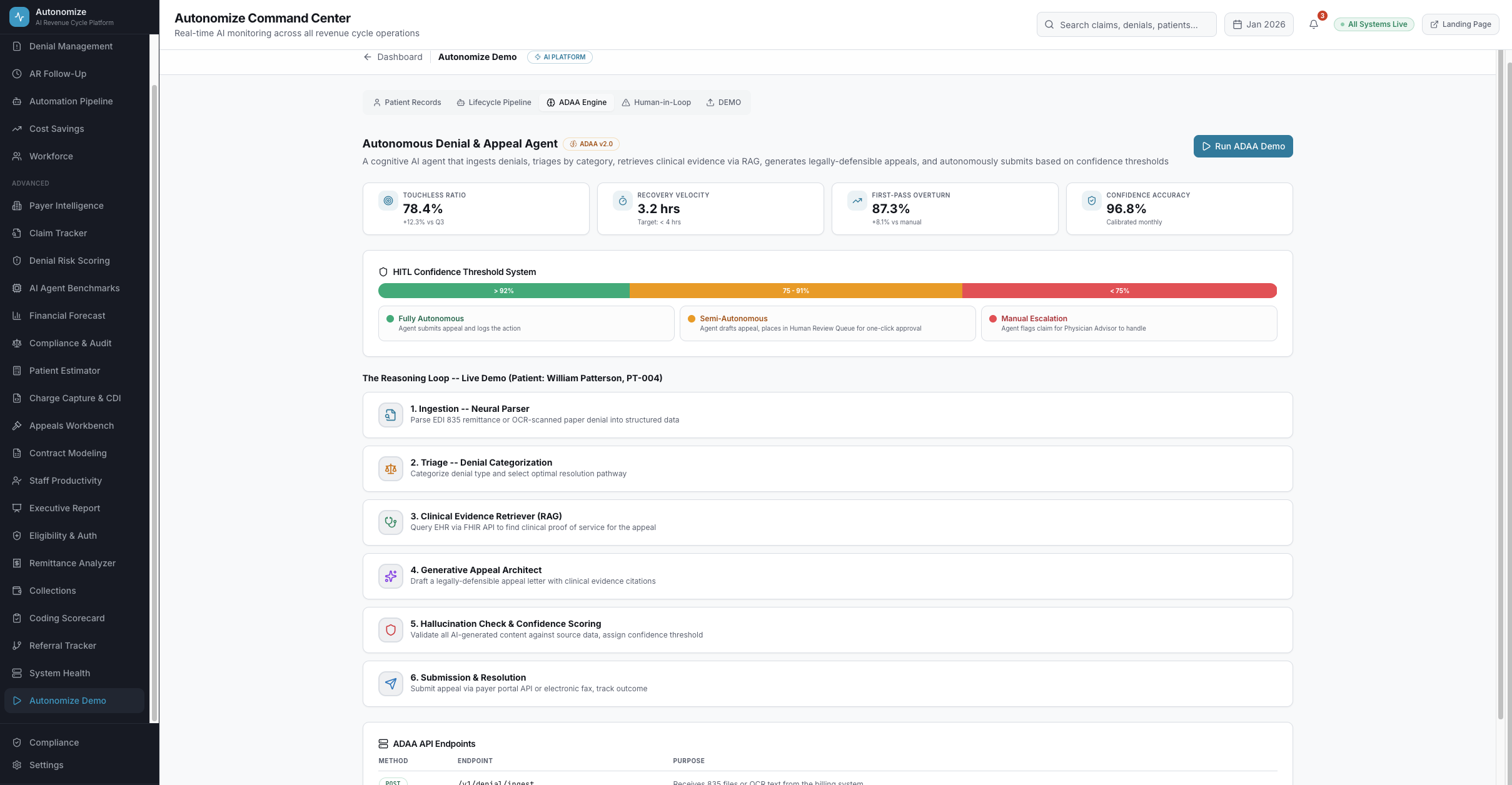
8 stationsAutonomous Denial & Appeal Agent
A cognitive AI agent that ingests denials, triages by category, retrieves clinical evidence via FHIR RAG, generates legally-defensible appeals, validates against hallucination, and submits autonomously.
Touchless Ratio
78.4%
Resolved without human opening the claim
Recovery Velocity
3.2 hrs
Denial received to appeal submitted
First-Pass Overturn
87.3%
Overturned on first attempt
Confidence Accuracy
96.8%
Predictions above 92% that overturned
Neural Parser
Ingests EDI 835 remittance or OCR paper denial, maps cryptic payer codes to actionable logic via LLM fine-tuned on 2.4M+ transactions
Triage Engine
Categorizes denial type (Medical Necessity, Prior Auth, Coding, etc.) and selects optimal resolution -- auto-correct or auto-appeal
Clinical RAG Retriever
Queries EHR via FHIR R4 (DiagnosticReport, DocumentReference) to retrieve bronchoscopy results, ABG values, physician notes
Appeal Architect
Generates legally-defensible appeal letter with clinical evidence citations, 42 CFR references, and payer-specific templates
Hallucination Guard
Validates every date, lab value, and clinical reference against EHR source. Assigns confidence score: >92% = fully autonomous
Auto-Submission
Files appeal via payer portal API. Result: 87.3% first-pass overturn, 3.2 hours denial-to-submission, $112K recovered per case
Confidence Threshold Zones
See the platform in action
7 dashboard views. Every metric drillable. Every AI decision auditable.
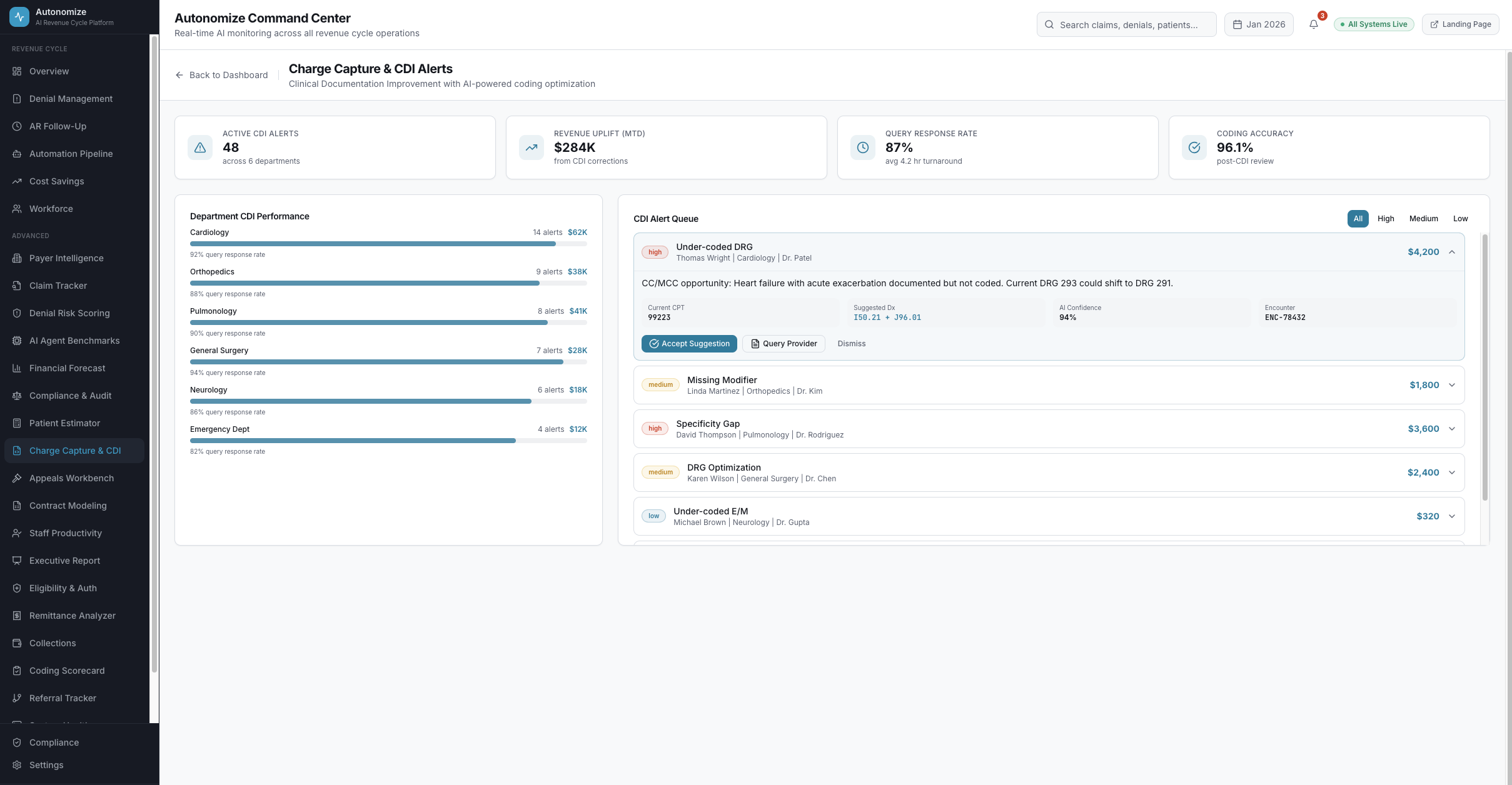
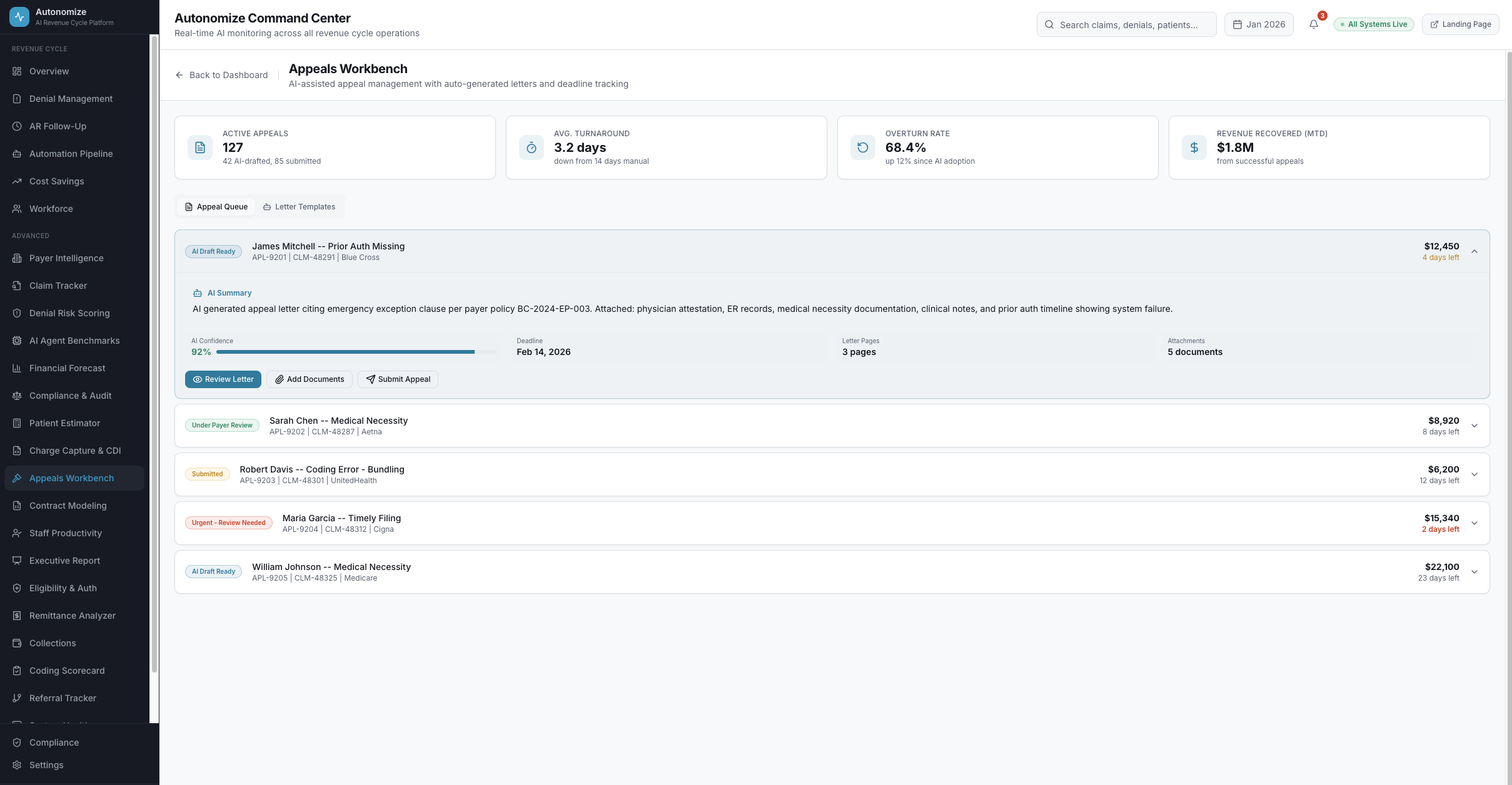
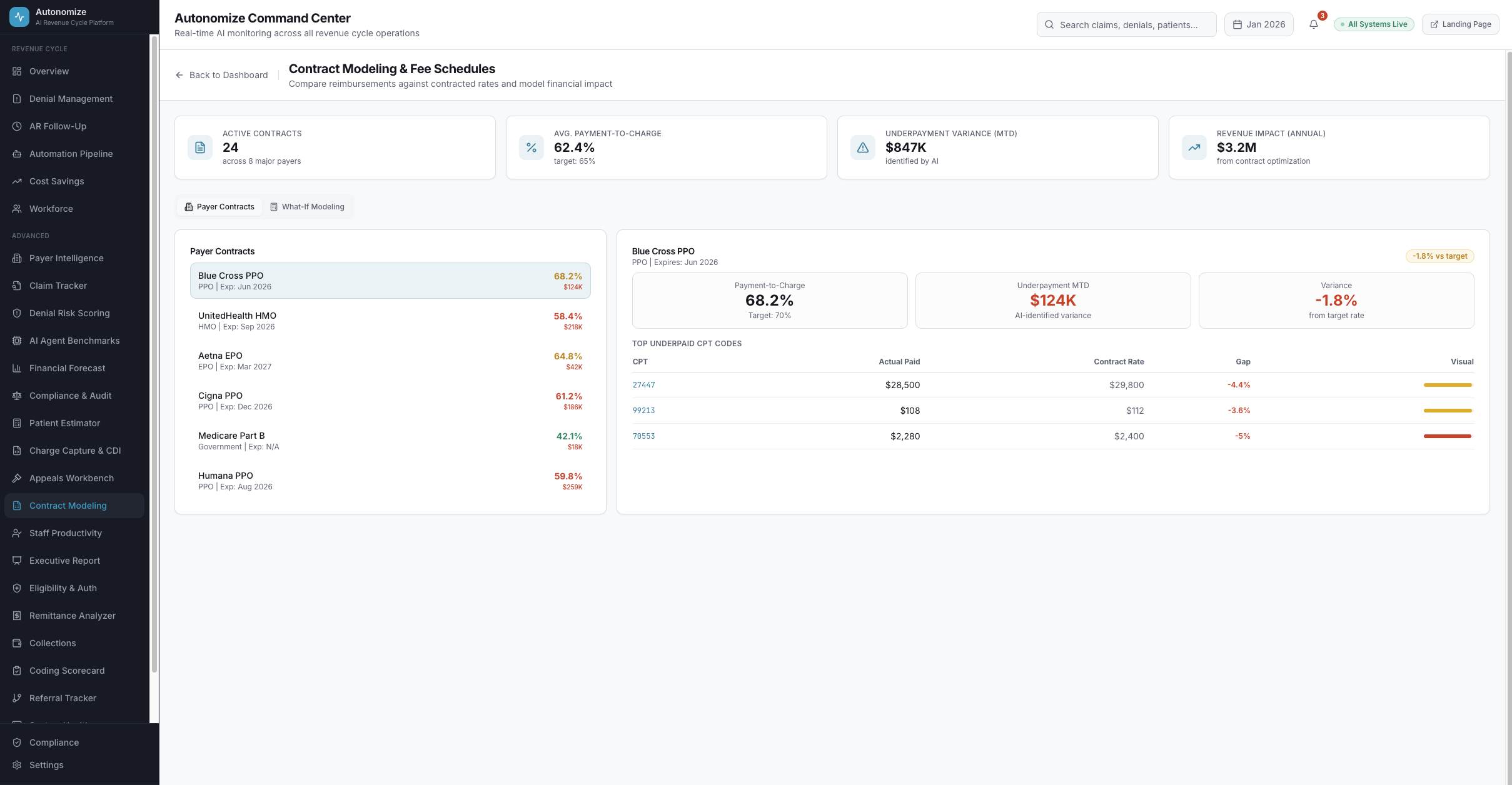
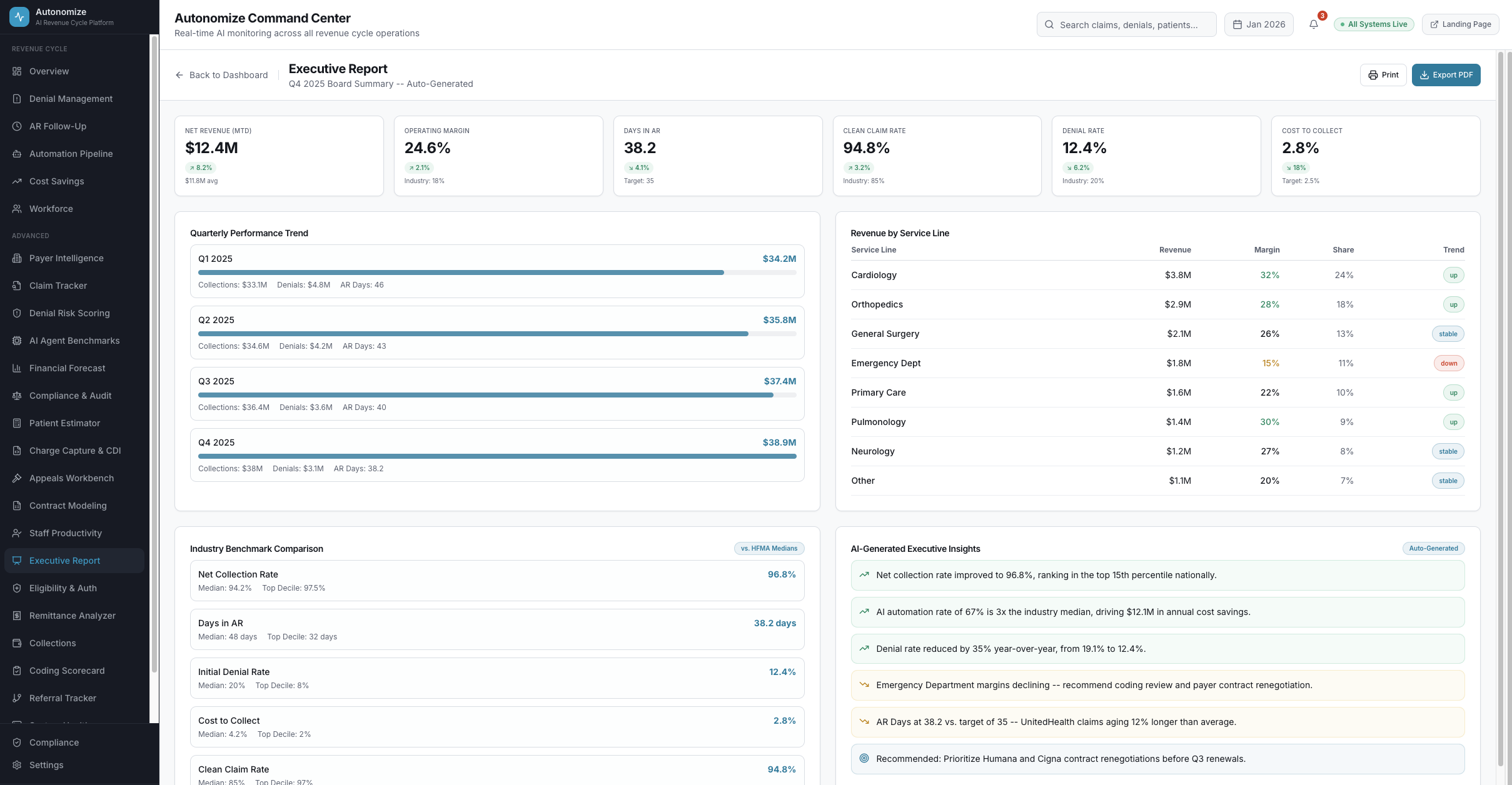
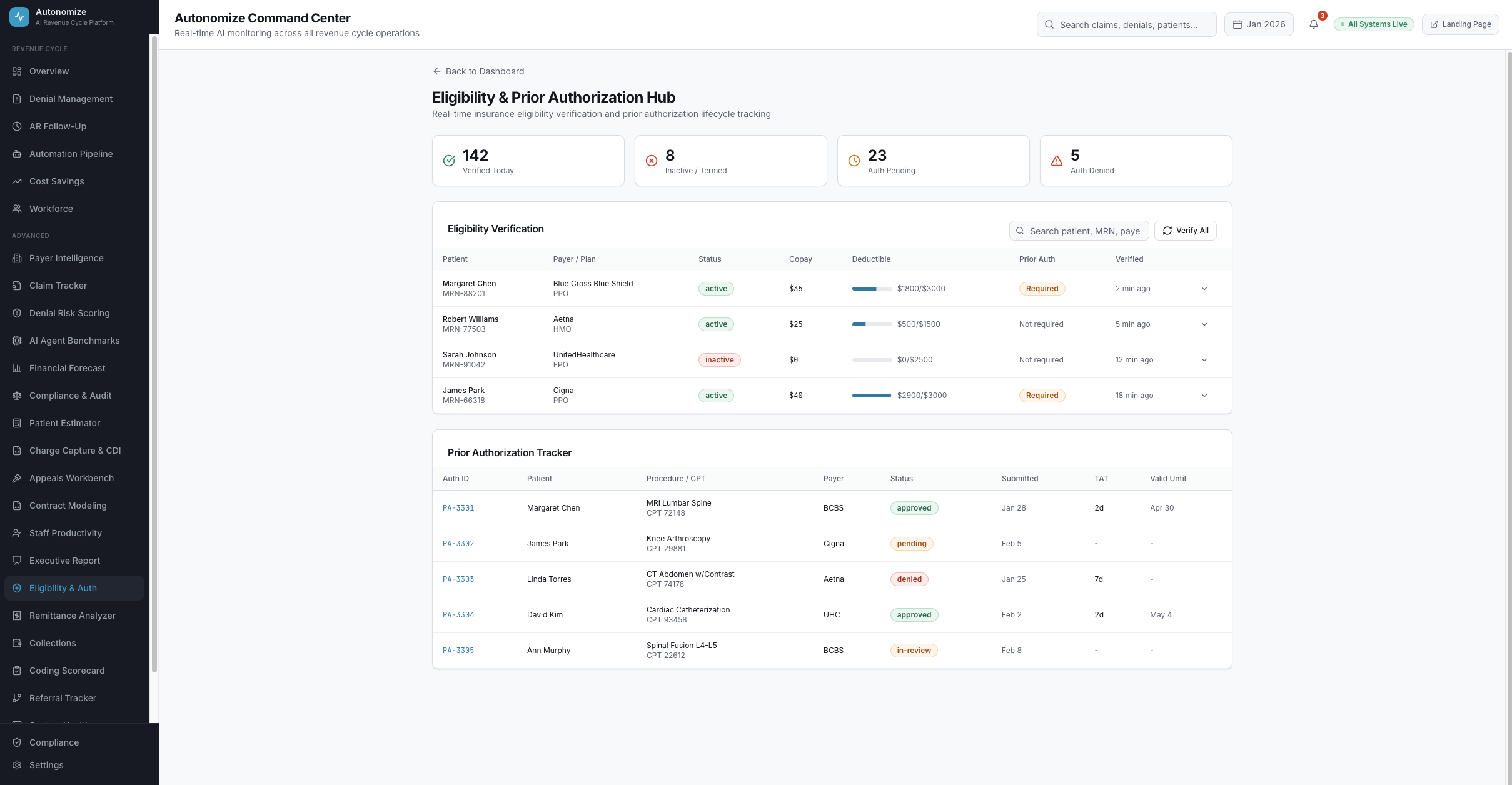
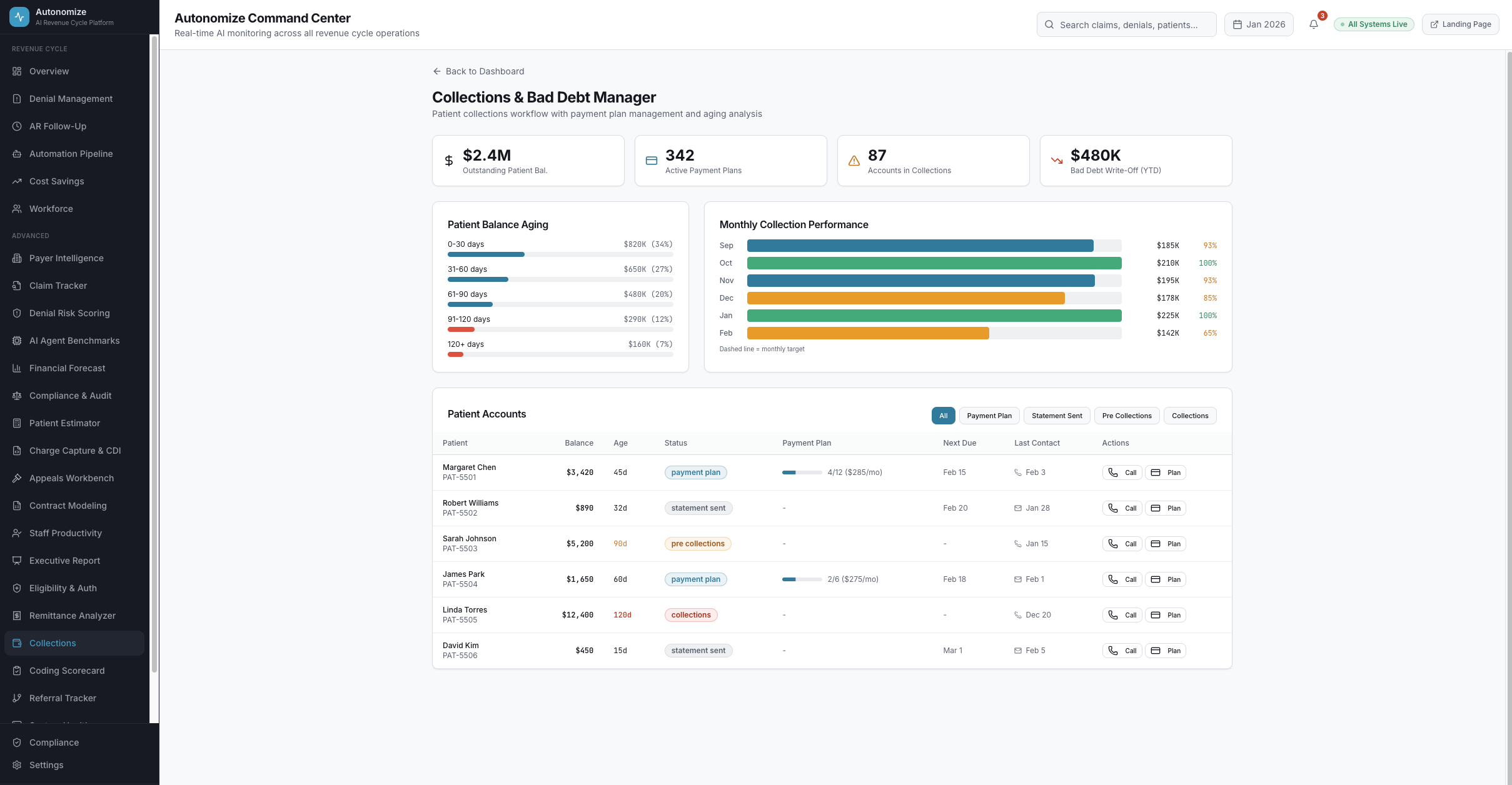
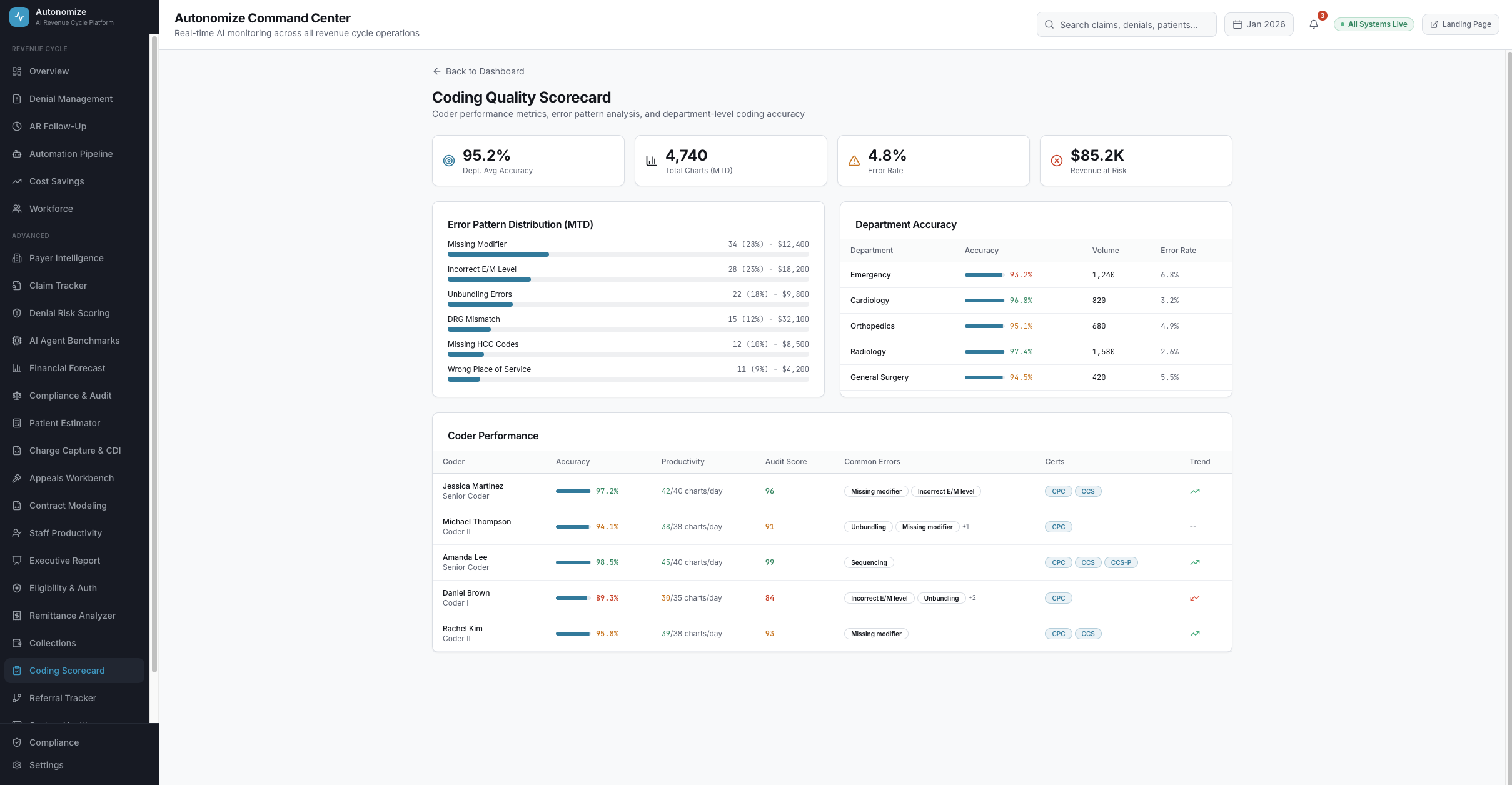
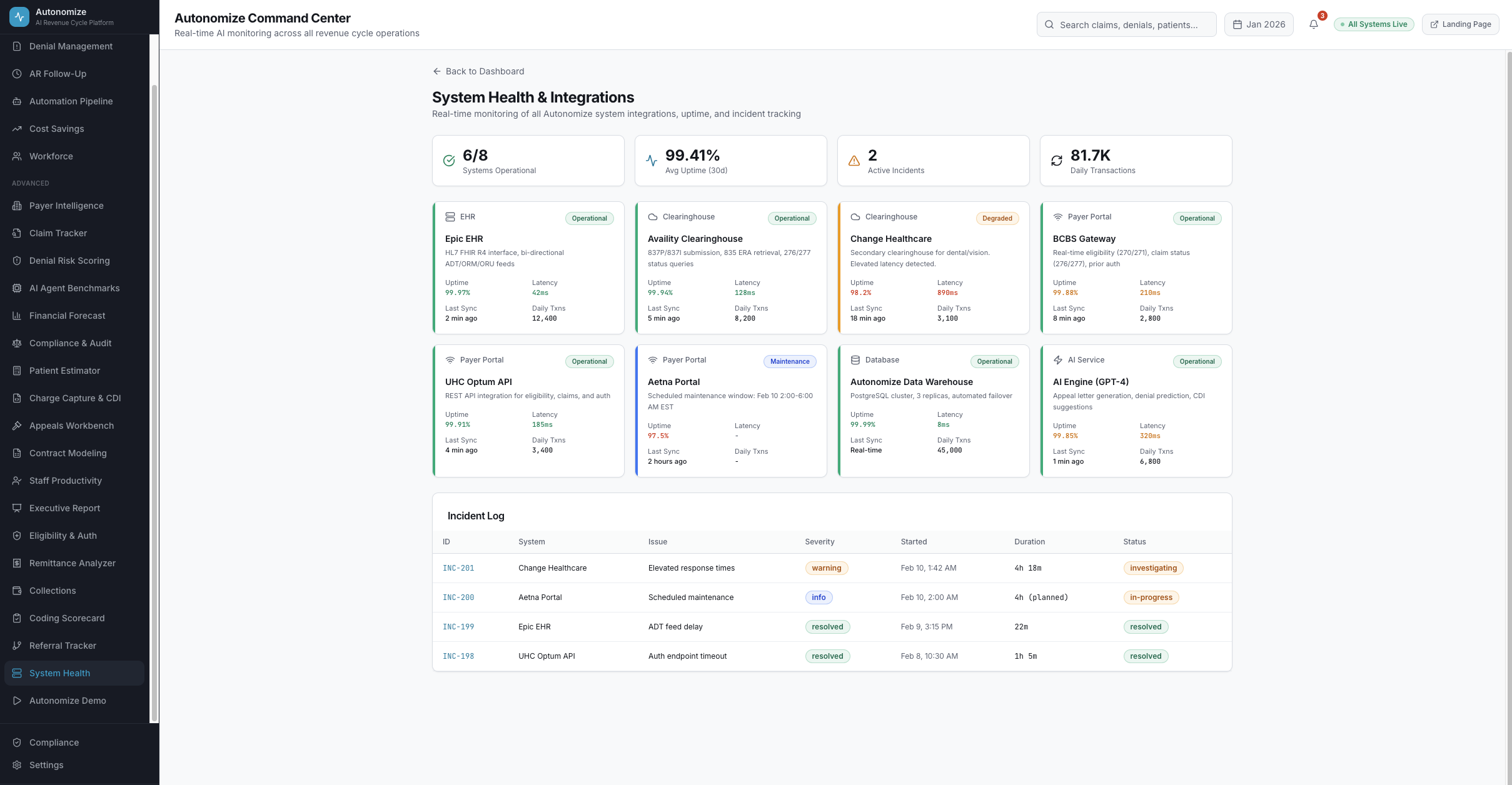
Real-time operations intelligence
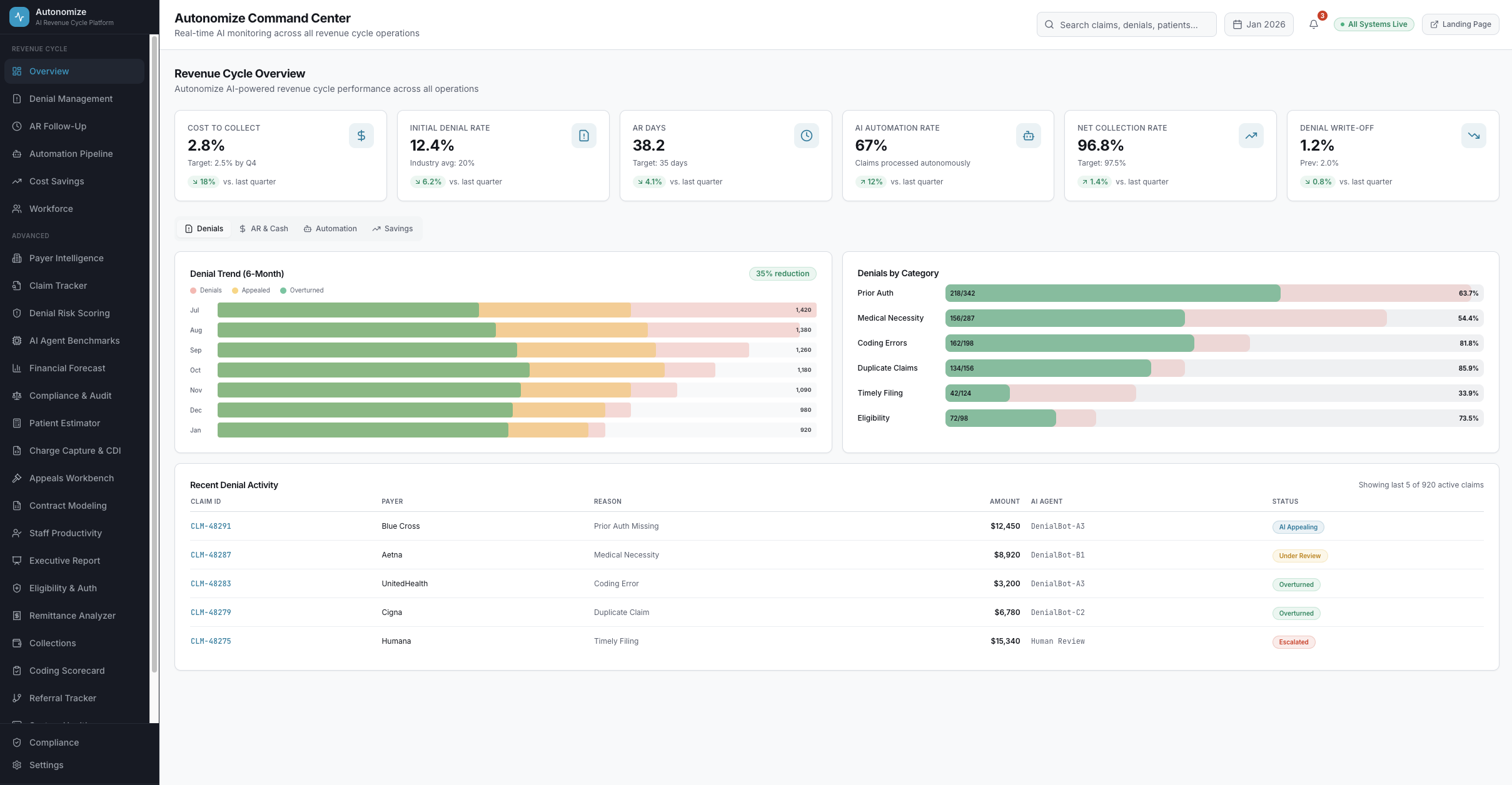
Revenue Cycle Overview
6 KPIs tracking cost to collect (2.8%), denial rate (12.4%), AR days (38.2), AI automation (67%), net collection (96.8%), and write-offs (1.2%). Denial trends, category breakdowns, and recent activity -- the entire revenue cycle in one view.
6 agents. 451K claims. Zero human touch.
Each agent is trained on millions of claims specific to its domain -- continuously improving with every transaction.
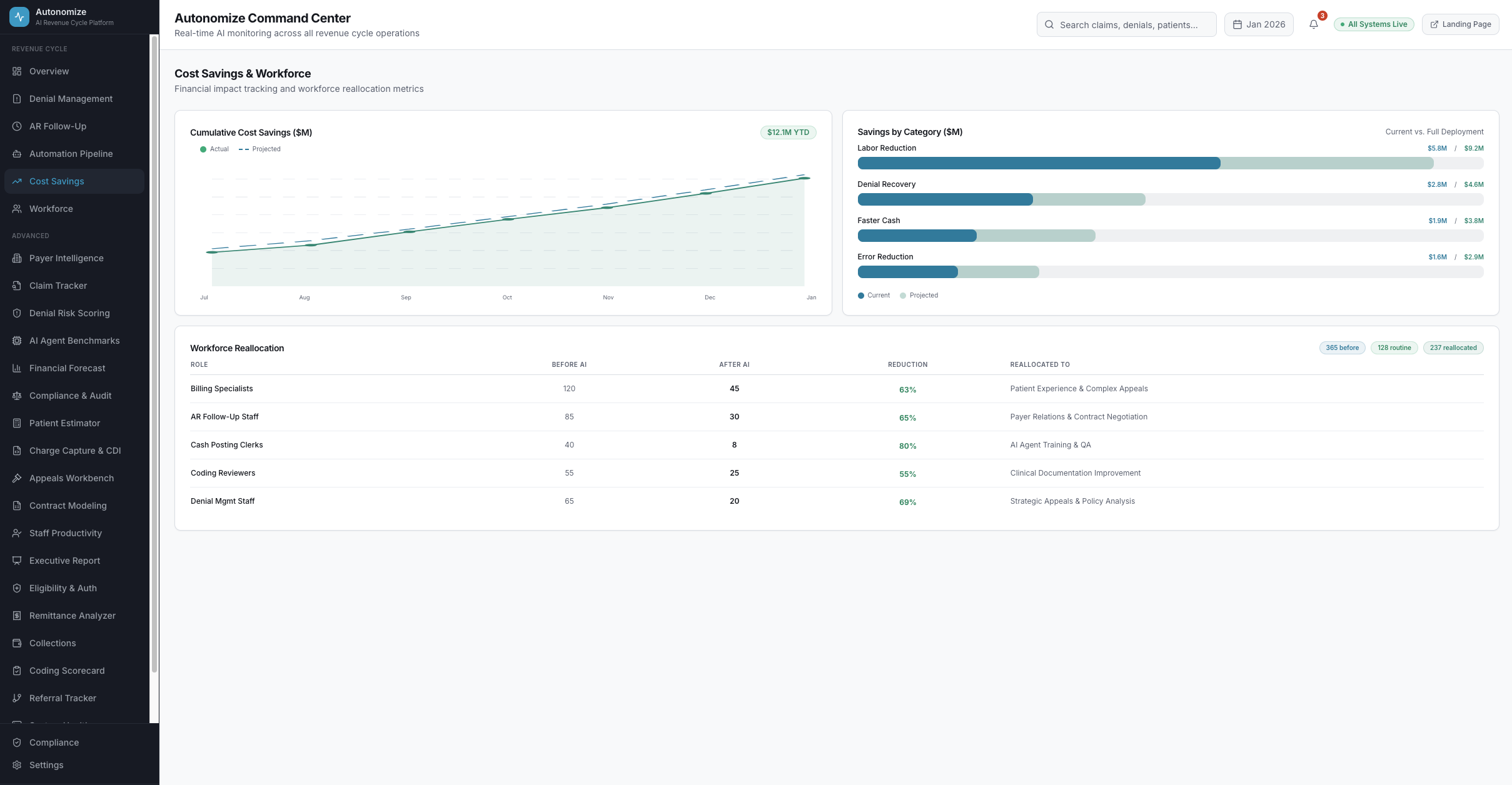
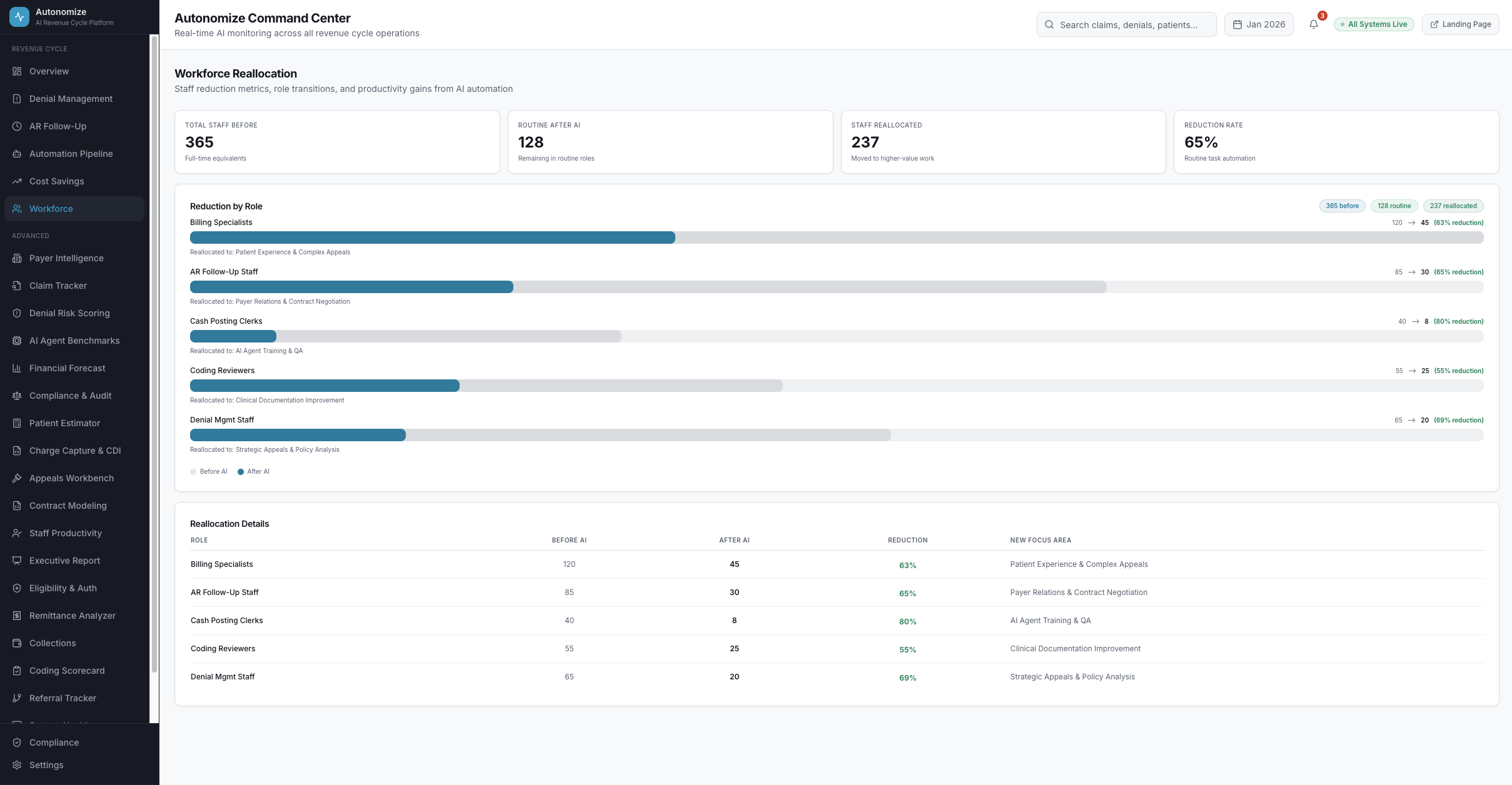
Not replacing humans. Elevating them.
365 staff performing routine billing tasks reallocated to 237 strategic roles -- patient experience, payer negotiation, clinical documentation improvement.
365
Before AI
128
Routine Tasks
237
Upskilled
Reallocated to: Patient Experience & Complex Appeals
Reallocated to: Payer Relations & Contract Negotiation
Reallocated to: AI Agent Training & QA
Reallocated to: Clinical Documentation Improvement
Reallocated to: Strategic Appeals & Policy Analysis
25+ dashboard modules
Every aspect of the revenue cycle has a dedicated intelligence view.
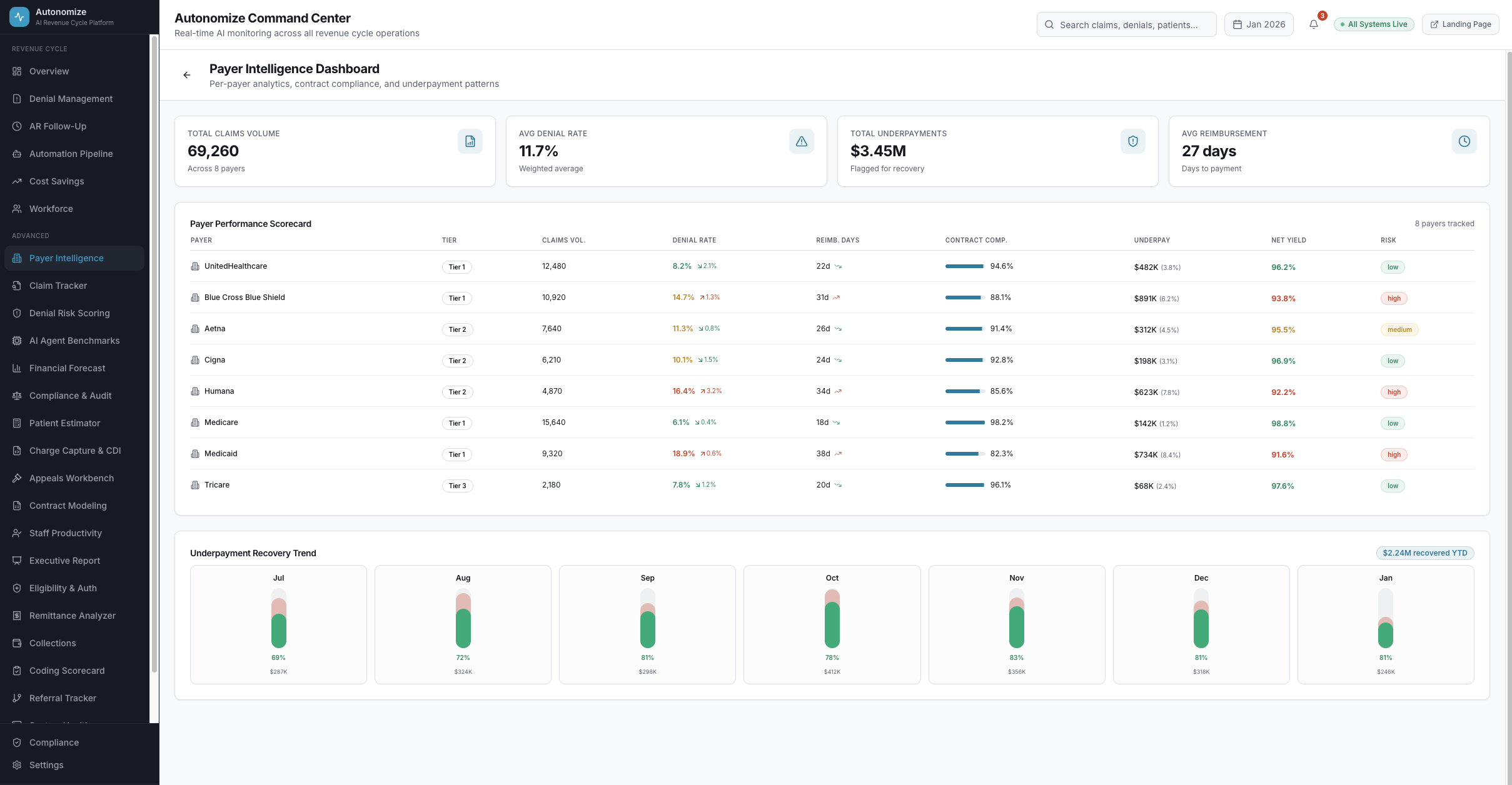
Payer Intelligence
Per-payer denial rates, appeal success rates, underpayment patterns, contract compliance
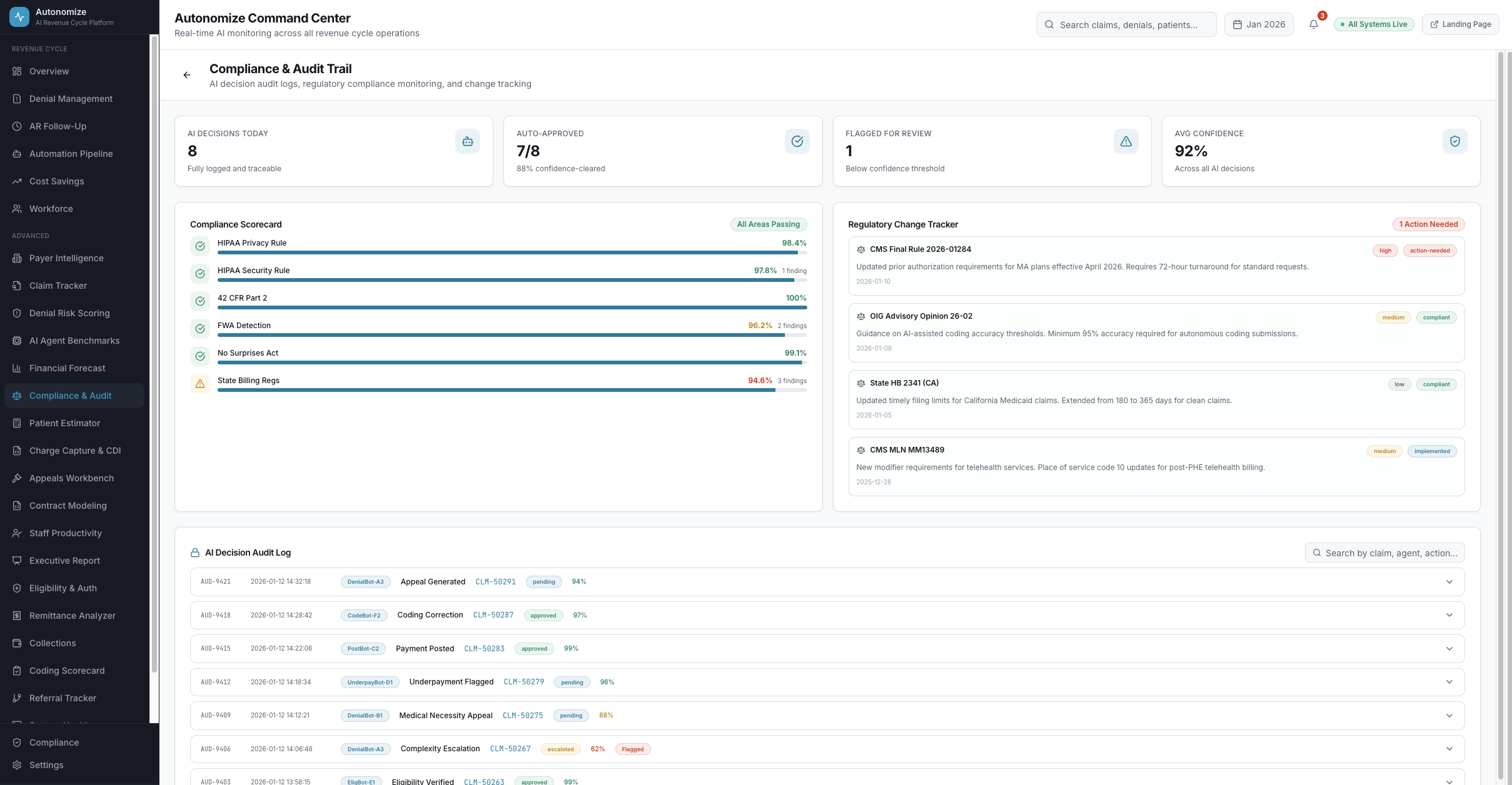
Compliance & Audit
AI decision audit trails, HIPAA compliance scoring, regulatory change tracking
Patient Estimator
Real-time OOP cost estimates using deductible status, contract rates, benefit accumulators
Charge Capture & CDI
AI-identified documentation gaps, DRG optimization, +$3,100 reimbursement uplift per case
Appeals Workbench
AI-drafted appeal letters, deadline tracking, payer-specific templates, bulk processing
Remittance Analyzer
ERA/EOB parsing, variance detection, underpayment flagging, $412K flagged today
Referral Tracker
Referral lifecycle management, authorization status, visit utilization tracking
System Health
Real-time integration status for EHR, clearinghouse, and payer portal connections
Deploy in weeks, not months
Connect
Integrate with your EHR, clearinghouse, and payer portals via HL7 FHIR, X12 EDI, and direct APIs. Native support for Epic, Cerner, Meditech.
Deploy
Pre-trained agents activate across your revenue cycle. Each learns your payer mix, contract rates, and denial patterns within days.
Scale
Real-time ROI tracking across every agent. Full visibility into automation rates, savings, workforce impact, and compliance scores.
Ready to eliminate revenue leakage?
See all 17 pipeline stations in action. Run a patient through the full revenue cycle and watch AI agents process every step autonomously.